by Emily Evans, O.D.
Dry, itchy, burning, blurry…Sound familiar? You may have Dry Eye Disease.
 It’s important to stay hydrated, right? We all know the recommendation, six to eight 8 ounce glasses of H2O per day. We carry around our water bottles and make sure to refill. So why aren’t we as concerned about hydrating our eyes? Our eyes need lubrication not only to feel comfortable, but also to see correctly. July is Dry Eye Awareness Month, and if you’re one of the 30 million Americans who suffer from this disease, you need to know how to get a handle on it.
It’s important to stay hydrated, right? We all know the recommendation, six to eight 8 ounce glasses of H2O per day. We carry around our water bottles and make sure to refill. So why aren’t we as concerned about hydrating our eyes? Our eyes need lubrication not only to feel comfortable, but also to see correctly. July is Dry Eye Awareness Month, and if you’re one of the 30 million Americans who suffer from this disease, you need to know how to get a handle on it.
Symptoms
Dry Eye Disease can mask itself in many ways: burning, grittiness, blurred vision, foreign body sensation, redness, itchiness, dryness (of course!), and even tearing. Additionally, if your vision changes when you blink, you may have dry eye.
Who Gets Dry Eye
Anyone can get Dry Eye Disease, but it becomes more common as we age. Women are two times as likely as men to get Dry Eye Disease, and the incidence increases after menopause. This can be attributed to hormones and lifestyle (such as cosmetic use). Anyone who uses the computer (yes, you reading this!) are more at risk for dry eye. When focusing on a digital screen, your eyes blink less and thus get dehydrated easier. After eye surgery, some people temporarily experience dry eye symptoms. Before or after LASIK, you may need a short-term course of dry eye treatment. Lastly, those contact lenses that you put in every day can actually dry your eyes out! Some people get so dry that they become contact lens-intolerant.
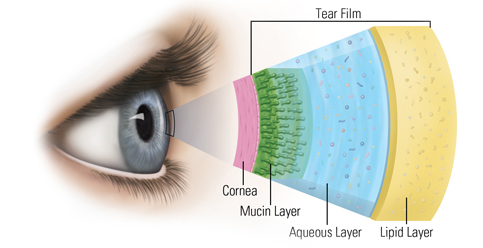
Tear Film Layers
Our tear film is made up of three important layers: first, the outermost lipid (oil) layer, then the aqueous (water) layer, and finally the bottom mucin layer. These three components help the eye stay lubricated, and believe it or not, affect our vision! An ocular surface with a normal and smooth tear film sees much better than a surface with a disorganized or poor tear film. Our eyes need all three layers to see correctly and to feel comfortable.
Forms of Dry Eye
There are two main forms of dry eye, categorized by what is not working correctly. The first is called Aqueous-Deficient Dry Eye, which means that your eyes are not producing enough of the water layer of tears. This is caused by a faulty lacrimal gland. Second, and most common, is called Evaporative Dry Eye or Meibomian Gland Dysfunction, which means that your eye can produce the water layer of tears, but those tears are evaporating too quickly to function. In this type, the oil layer is not being produced correctly by the Meibomian Glands, thus leaving the water layer exposed to the environment.
Medications and Conditions that Affect Dry Eye
If you’re like me and Nashville allergies are taking over your sinuses, you’re probably using an oral antihistamine. Great! But wait, these can actually make your eyes more dry. What? No, that’s not a reason to stop using your pills (you’d be more miserable!) but it is cause to use some form of dry eye treatment. Other medications like antidepressants and diuretics are also culprits of causing dry eye. Consult your eye doctor for a dry eye evaluation if you are on any of these drugs.
Autoimmune and inflammatory diseases such as Sjogren’s Syndrome, Rheumatoid Arthritis, Rosacea, and Lupus can also cause Dry Eye Disease. If you have one of these conditions, it’s best to consult with your eye doctor as soon as possible about initiating treatment. Sjogren’s Syndrome is a major dry eye culprit; it causes moisture-producing glands in the body to stop working. If you have a dry mouth and dry eyes, you may consider getting tested for Sjogren’s Syndrome.
What to Do if You Suffer from Dry Eye
Avoid direct air or wind toward your eyes. This means turning off that ceiling fan at night, directing your car’s A/C vents away from your face, and wearing sunglasses outside in the wind (yes, it helps!). If you are traveling, make sure to double up on artificial tears if you plan on flying. Planes are notorious for greatly exacerbating dry eye; the lack of moisture in such a closed area really dehydrates your ocular surface.
Treatment
 Dry Eye Disease is a chronic and progressive disease; and while it is not curable, it is manageable. Drugstore “eye drops” or a bottle that claims “get the red out” are the most commonly sought remedies, but are not often the best choices. How do you know what to use? It’s best to have an examination by your eyecare provider to find out what you need.
Dry Eye Disease is a chronic and progressive disease; and while it is not curable, it is manageable. Drugstore “eye drops” or a bottle that claims “get the red out” are the most commonly sought remedies, but are not often the best choices. How do you know what to use? It’s best to have an examination by your eyecare provider to find out what you need.
Your eye doctor may start with an over the counter lubricating drop or artificial tear, used three or four times a day for mild dry eye. With more frequent use, it is recommended to choose a preservative-free tear. Gel or ointment tears are used at bedtime to coat the eye’s surface as you sleep. Hot compresses are usually recommended for people with Evaporative Dry Eye to help unclog the oil glands. Studies have shown that omega 3 fatty acids (fish oil) help reduce dry eye symptoms, and so your doctor may start you on these supplements.
As the severity of Dry Eye Disease increases, treatments can vary. There are two prescription eye drops for Dry Eye Disease, cyclosporine and lifitegrast. Your eyecare provider may start treatment with these if you do not have relief with over the counter drops. Temporary or permanent punctal plugs are sometimes utilized to block the tear duct in order to keep tears on the eye longer. Other procedures like lid scrubbing (debridement) or lid expression (unclogging) can be done in office to help your tears function better.
Loden Vision Dry Eye Clinic Treatment
Loden Vision is happy to offer FDA-approved Lipiflow, a thermal pulsation procedure that works to heat and unclog the Meibomian Glands to restore secretion of lipid tears. Seventy-nine percent of dry eye sufferers in a clinical study noticed long-term improvement in their symptoms after Lipiflow. We also offer Blephex, a lid scrubbing procedure that functions as a routine clean for your eyelids. Just as you go (or should go!) to the dentist to get your teeth cleaned every 6 months, it is recommended to deep clean your eyelids and lashes every 6 months to prevent exacerbation of Dry Eye Disease.
What next?
If you’re tired of the dry, itchy, burning, blurry feeling of Dry Eye Disease, it’s time to schedule an appointment with our Dry Eye Clinic specialist. Don’t be left high and dry (pun definitely intended!); call us today!


